About Epilepsy

What Is Epilepsy?
Epilepsy is the tendency to have recurrent seizures. Using the most commonly used definition, having one seizure does not meet criteria for having epilepsy.
In contrast, having 2 or more seizures in your life does meet criteria for epilepsy. “Do I have epilepsy?” is a very common question at our clinic. This question is even asked by patients who have had epilepsy for many years. Often times, patients are feeling stressed about the diagnosis of epilepsy. A clear description of what epilepsy is all about can be very helpful for patients to better understand the diagnosis. A clear explanation may significantly relieve stress. We will often review the many different types of epilepsy. Patients can develop epilepsy at any age. Patients with epilepsy run the gamut in terms of physical and mental abilities. Judges, doctors, writers, musicians, artists, athletes, business leaders and teachers have successful individuals with epilepsy within their ranks.
There may be clinical situations where a patient may have two seizures in their life and not have epilepsy. The key is whether or not the seizures are provoked by a temporary condition. An example is a patient with diabetes who has their glucose drop to dangerously low levels. Extremely low glucose levels can trigger seizures. Such a patient could have two or more seizures and still not meet criteria for epilepsy—because the seizures were provoked. In contrast, patients with epilepsy have an underlying tendency to have recurrent seizures, even without any obvious provocation.
What Is a Seizure?
A seizure is a temporary change in the electrical activity of the brain. In the normal state, the cells on the surface o f the brain (the neurons) communicate and function by an organized flow of electricity. In a seizure, excessive electrical charge occurs—this excessive electricity results in abnormal brain activity. This abnormal activity will lead to the symptoms of the seizure.
An example will be useful to clarify this concept. As many people know, the right side of the brain controls the left side of the body. In the right front part of the brain, there is an area that controls left hand function. When I think, “move my left hand”, a smooth and organized flow of electricity occurs in the right front part of my brain—resulting in the movement of my left hand. Now imagine that a swarm of electrical activity is occurring in the right front part of my brain. Picture a major electrical power surge! The abnormal electrical activity would result in abnormal left hand movements. This would often result in jerking in my left hand. This is what a seizure is—abnormal electricity in the brain causing abnormal movements or other symptoms.
Now, let’s say the seizure activity in the above example became more widespread. Instead of being just in my right frontal region, it spread to involve my entire brain! You can imagine that if my whole brain was affected by excessive electrical activity, then the effects on my body would be dramatic- this could result in a “grand mal” seizure. A “grand mal” seizure is where a person collapses to the ground and has whole body shaking activity.
Normal brain function occurs through an organized flow of electricity from the neurons on the surface of the brain. A seizure is like a power surge of electricity in the brain. The abnormally excessive electrical activity can disrupt brain function and may cause confusion, jerking and/or collapsing—all symptoms of a seizure.
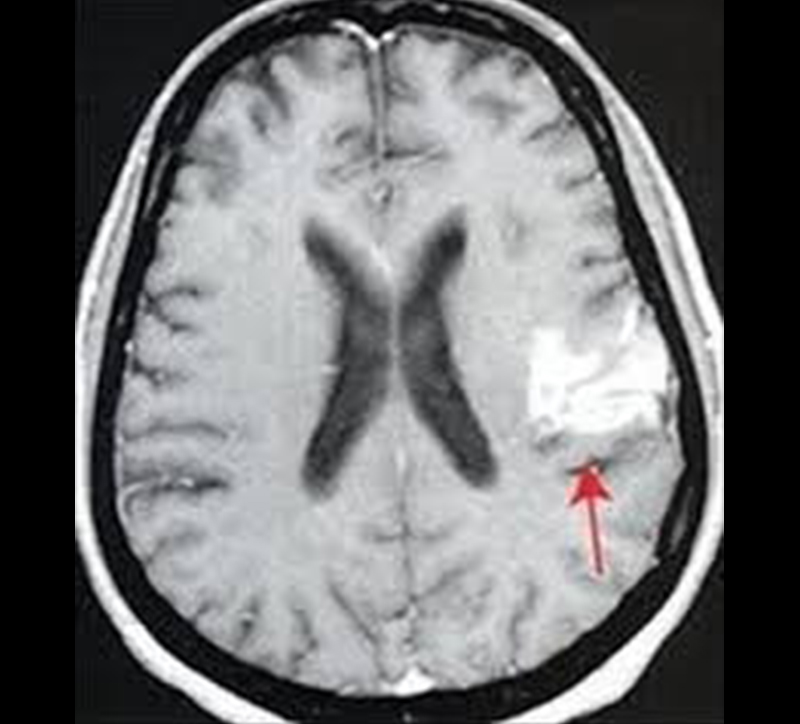
What Causes Seizures?
This is an extremely important question. The doctor’s job is to do the detective work to answer this question as accurately as possible. Identifiable causes of seizures are typically due to conditions that disrupt the normal flow of electricity in the brain. Conditions such as head-trauma, stroke and infection can cause scarring on the brain. This will disrupt the wiring between the brain’s cells (neurons). This will in turn cause the potential for abnormal electrical charge from those cells. Excessive electrical charge from neurons can produce seizures.
The most common cause of epilepsy that begins in childhood is birth related issues. In adults, stroke is the most common reason to develop epilepsy. Stroke accounts for just over 10% of new-onset epilepsy and approximately one-third of cases with an identified cause. Brain tumors (approximately 6%) and Alzheimer’s Disease/other dementias (approximately 7%) are other common causes. Depending on where you live in the world, infection may be a very common, if not the most common, cause of epilepsy.
Certain conditions, if they apply to you, can dramatically increase your risk of seizures. For example, a penetrating head injury, such as a bullet piercing the brain, can increase the risk of developing epilepsy 500 times (compared to the general population). In those patients with encephalitis (a severe brain infection), > 20% of patients may develop epilepsy.
Despite extensive work-up, including history, physical examination, EEG, MRI and blood testing, a large percentage of patients still do not have an identified cause for their seizures. This is in some ways reassuring—at least the patient does not have a stroke, tumor or other life-threatening illness. On the other hand, the patient and family are often very frustrated about not getting answers. Most large studies report that the cause of a patient’s epilepsy is unknown in greater than 50-60% of cases. As brain imaging and other technologies improve, it is hoped that the “unknown” category shrinks to as close to zero as possible. One area of very hot research is in the genetics of epilepsy—this may explain a big part of the “unknowns.”
